Waking up with a shoulder that feels like it's on fire or a knee that throbs every time you stand up is frustrating. Most people just call it "joint pain," but there is a big difference between a problem in your tendons and a problem in your bursae. If you treat one like the other, you might actually make the injury worse. In fact, using a cortisone shot on a weakened tendon can sometimes do more harm than good, while the same shot might be a lifesaver for a swollen bursa. Understanding exactly which structure is inflamed is the only way to get back to your normal routine without a relapse.
The Basics: What is Actually Happening?
To fix the pain, you first have to know what is broken. Your joints aren't just bones meeting; they are surrounded by a complex support system. Bursitis is the inflammation of the bursae, which are small, fluid-filled sacs that act as cushions between bones, tendons, and muscles . Think of them like tiny hydraulic pillows that stop your tissues from rubbing raw against each other. When these sacs get irritated-usually from repetitive pressure or a sudden hit-they fill with too much fluid and swell, causing a dull, aching pain.
On the other hand, Tendinitis is the inflammation or irritation of a tendon, the thick fibrous cord that anchors your muscle to your bone . While bursitis is about cushioning, tendinitis is about tension. When you overwork a muscle or use a repetitive motion for years, the tendon develops microscopic tears. If the body can't keep up with the repairs, the area becomes inflamed, leading to a sharper pain that usually spikes when you actually move the joint.
How to Tell Them Apart
It is easy to confuse the two because they often happen in the same spot. For instance, about 65% of people with shoulder issues actually have both subacromial bursitis and rotator cuff tendinitis at the same time. However, the Bursitis and Tendinitis distinction usually comes down to how the pain behaves.
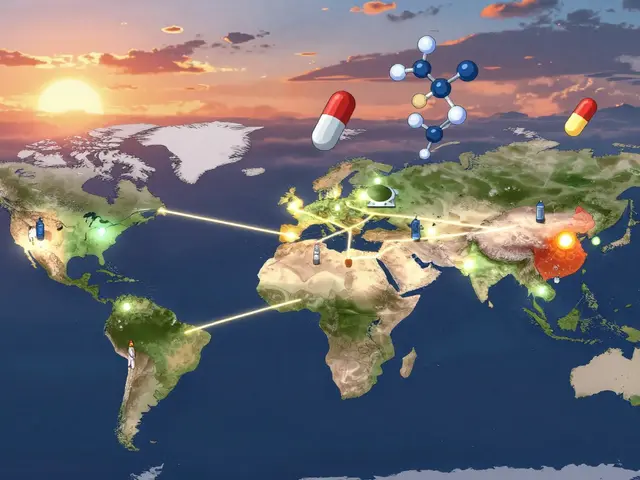
If you have bursitis, the pain is often diffuse. You might feel a general "warmth" or ache around the joint. A classic sign is pain that gets worse at night when you lie directly on the affected area. For example, if you can't sleep on your side because your hip or shoulder feels like it's pressing into a bruised balloon, that is a strong signal for bursitis.
Tendinitis is different. The pain follows a specific path-the line of the tendon. It is most intense during the actual movement that stresses that tendon. If your ankle screams only when you push off your toes to walk, you are likely dealing with Achilles tendinitis. While bursitis feels like pressure, tendinitis feels like a pull.
| Feature | Bursitis | Tendinitis |
|---|---|---|
| Primary Structure | Fluid-filled sac (Bursa) | Fibrous cord (Tendon) |
| Pain Type | Dull, aching, diffuse | Sharp, localized, "pulling" |
| Trigger | Direct pressure/friction | Repetitive motion/tension |
| Night Pain | Common when lying on the joint | Less common; linked to movement |
| Recovery Time | Typically 4-6 weeks | Often 12-16 weeks |
The Recovery Roadmap: From Ice to Exercise
Recovery isn't a one-size-fits-all deal. The American College of Rheumatology suggests a stepped approach. You don't start with surgery; you start with the basics. The first 7 to 10 days are about "calming the storm." This means activity modification-stop doing the thing that caused the pain-and using ice therapy. A great pro tip from experienced patients is using a frozen water bottle to roll out the area, which provides both cold therapy and a gentle massage.
Once the initial swelling goes down, the path for each condition diverges. For bursitis, the goal is to remove the pressure. Rest and anti-inflammatories (NSAIDs) usually do the trick within a month. But for tendinitis, simply resting is a mistake. Tendons need a specific kind of stress to heal. This is where Eccentric Strengthening is a rehabilitation technique where the muscle lengthens under tension, such as slowly lowering your heel off a step . This process realigns the collagen fibers in the tendon, making it stronger and less likely to tear again.
If conservative methods fail, doctors might suggest injections. However, the evidence shows a clear divide in success rates. Cortisone shots work wonders for bursitis-around 78% of patients see significant short-term relief. For tendinitis, the success rate is much lower (around 52%), and some people actually feel worse because cortisone can weaken the tendon's structural integrity over time.
Common Pitfalls and Misdiagnosis
One of the biggest mistakes people make is self-diagnosing as "rotator cuff problems" and jumping straight into heavy strengthening exercises. If you have acute bursitis, aggressive exercise can act like sandpaper on a wound, prolonging your recovery by weeks. You have to wait for the inflammation to subside before you start building strength.
Another trap is over-relying on MRI scans. It sounds crazy, but about 40% of healthy adults over 50 have signs of bursitis or tendinitis on an MRI without actually feeling any pain. This is why a clinical exam-where a doctor checks your range of motion and feels for localized tenderness-is more important than a picture. If the image says you have a problem but you feel fine, you don't need treatment.
Modern Alternatives and Future Tech
If you've tried physical therapy and it's not working, there are newer options. Platelet-Rich Plasma (PRP) is a treatment where a patient's own blood is processed to concentrate platelets and then injected into the injury . For chronic tendinitis, PRP has shown better long-term results than corticosteroids, with a 67% improvement rate at the six-month mark. It's more expensive, but it aims to actually repair the tissue rather than just masking the inflammation.
We are also seeing a shift toward wearable tech. New motion-tracking algorithms in smartwatches are becoming accurate enough to spot the exact movement patterns that lead to tendinitis. In the near future, your watch might warn you that your wrist angle during typing is putting you at risk for inflammation before you even feel the first twinge of pain.
Can I treat both with the same exercises?
Not exactly. While gentle range-of-motion stretches help both, tendinitis requires specific eccentric loading (lengthening the muscle under weight) to heal. Doing these heavy loads during the acute phase of bursitis can actually increase inflammation and slow down your recovery.
How long does it actually take to heal?
Bursitis typically resolves in 4 to 6 weeks with rest and anti-inflammatories. Tendinitis is a slower process; a full course of structured rehabilitation often takes 12 to 16 weeks. Patience is key here-rushing back into sports often leads to a chronic condition called tendinopathy.
Are cortisone shots safe?
They are effective for short-term pain, especially in bursitis. However, medical guidelines recommend limiting them to 2-3 injections per year. Overusing them can weaken the tendons and ligaments, making the joint more prone to future injuries.
What is the "pain monitoring rule"?
When doing rehab exercises, you should aim for "therapeutic discomfort." On a scale of 1 to 10, your pain should stay between 2 and 3. If the pain hits 5 or higher, you are pushing too hard and may be causing more damage to the tissue.
When should I see a surgeon?
Surgery is actually rare for these conditions, required in fewer than 5% of cases. You should only consider it if you've tried conservative management and PRP for several months without improvement, or if the inflammation has led to a full tendon tear.
Next Steps for Your Recovery
If you're currently in pain, start by tracking your triggers. Does it hurt when you push off your foot, or does it hurt when you lie on your side? If it's the former, look into a physical therapist who specializes in eccentric strengthening. If it's the latter, focus on reducing direct pressure and using ice massage.
For those in repetitive jobs-like musicians or construction workers-the best medicine is prevention. Modify your workstation or use knee pads to stop the cycle of friction. Remember, the goal isn't just to stop the pain today, but to change the movement patterns that caused the inflammation in the first place.